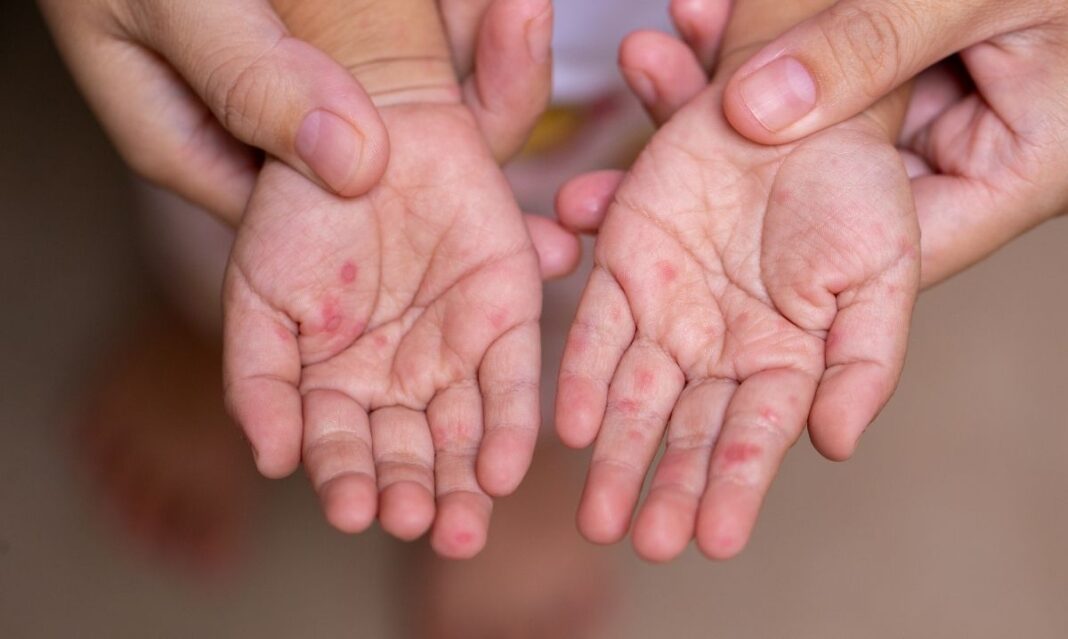
Your toddler won’t eat breakfast. By lunchtime, they’re running a fever. Then you spot it: tiny red blisters dotting their palms and the soles of their feet. It could be hand, foot and mouth disease, the viral illness that sweeps through daycares every year.
What is hand, foot and mouth disease?
Hand, foot and mouth disease is an illness caused by a group of viruses called enteroviruses. The most common culprits are coxsackievirus A16 and enterovirus A71, though several different viral strains can cause the infection.
These viruses are common in places where young kids congregate, such as daycares and elementary schools. While the disease primarily affects young children, anyone can get it, including teenagers and adults. There are several different viruses that cause it, so you can also get it multiple times.
Symptoms of hand, foot and mouth disease
The name gives away the most obvious symptoms, but the illness starts in the mouth before spreading elsewhere. The first sign is often that a young child will refuse to eat because mouth sores — which can form on the gums, inner cheeks and tongue — are causing them pain. After that comes the fever, usually around 101 degrees Fahrenheit, followed by the visible rash.
The hand, foot and mouth rash appears as small red spots or blisters that can show up on:
- Arms and legs
- Buttocks
- Palms of the hands
- Soles of the feet
While the mouth lesions typically hurt, the skin lesions aren’t usually painful or itchy. That’s one way we can distinguish it from other rash illnesses like chickenpox.
How does hand, foot and mouth spread?
Hand, foot and mouth disease is highly contagious, and spreads through:
- Direct contact: With an infected person’s saliva, fluid from blisters or stool (like when changing a child’s diaper).
- Fecal-oral transmission: Which means touching a surface contaminated with fecal germs and then eating or touching your mouth.
- Respiratory droplets: When an infected person coughs or sneezes
Young children are the main spreaders of hand, foot and mouth because they drool, put their hands and other things in their mouths, and may not yet know how to wash their hands properly. The virus can also live in stool for up to four weeks after infection.
The incubation period (the time between exposure and the first symptoms) is typically three to five days, but it can range from two to seven days. If your child was exposed at a party and seven days have passed without symptoms, they probably won’t get it. But if it’s only been two or three days, watch for signs.
What’s the best treatment for hand, foot and mouth disease?
There’s no specific medication to treat hand, foot and mouth disease. Because it’s a virus, antibiotics won’t help — and giving them when not needed could contribute to antibiotic resistance. But there are ways you can help your child heal and avoid serious complications, including:
- Focus on fluids: Your child may refuse to drink, which is a common complication, but it’s important to keep them hydrated. Try offering popsicles, electrolyte drinks for kids, give small, frequent sips of water or milk, serve yogurt, applesauce or other soft, soothing foods that contain water, and avoid acidic or spicy foods that may irritate mouth sores
- Control pain with medications: If your pediatrician gives the go-ahead, your child can take acetaminophen (Tylenol) or ibuprofen (Motrin). However, steer clear of numbing gels or other topical medicines. Children can have allergic reactions or absorb too much medication through the sores, and that can be dangerous.
Should I call the doctor?

If your child seems very ill or you’re unsure whether they need to be seen, contact your pediatrician. Luckily, most cases of hand, foot and mouth disease go away on their own. Children can return to school or daycare once they’ve been fever-free for 24 hours without medication and their blisters have dried.
However, contact your child’s pediatrician if you see red flags such as:
- Fever that persists beyond a few days
- Rash that becomes more widespread or severe
- Signs of dehydration, such as dry mouth, no tears or decreased urination
- Symptoms that get worse or don’t improve after 10 days
While rare, hand, foot and mouth disease can occasionally lead to serious complications, including viral meningitis or encephalitis. Seek immediate medical attention if your child experiences:
- Severe headache or stiff neck
- Difficulty breathing or chest pain
- Extreme drowsiness or confusion
- Seizures
Preventing hand, foot and mouth disease
Good hand hygiene is the best way to keep this nasty bug away from you and your kids. But even if you’re a diligent handwasher, there’s no guarantee that you’ll never get it. You can reduce your risk if you:
- Avoid close contact with infected individuals.
- Disinfect toys and surfaces regularly.
- Wash hands thoroughly after diaper changes.
This content is sponsored by Henry Ford Health. At Henry Ford Pediatrics, we are committed to creating the highest quality of life for all children. Learn more about our pediatric primary care and specialty services at henryford.com/pediatrics.